Losing a tooth in your 30s or 40s can feel like a small problem at first, but it starts a chain reaction beneath the surface: bone around the missing tooth begins to shrink, neighboring teeth shift, and your bite and facial structure can change.
Act quickly to prevent progressive bone loss and preserve both long-term oral health and the options available for reliable restorations. Replacing a missing tooth early gives you the best chance to stop bone loss, avoid more complex surgery later, and keep more predictable, less costly treatment options open.
This article explains how tooth loss causes bone resorption, what can happen if you delay treatment, and the practical solutions—like timely implants or prosthetics—that help protect your jaw, function, and appearance, especially if you are considering bone grafting for dental implants in Greenville SC.
Understanding Tooth Loss and Bone Loss in Your 30s and 40s
You can lose a tooth for many reasons in early adulthood, and the jawbone beneath that tooth starts to change quickly without the root’s stimulation. Early action preserves bone volume, keeps adjacent teeth stable, and makes future restorations simpler and more predictable.
Causes of Missing Teeth in Early Adulthood
Tooth decay and untreated cavities remain common causes of tooth loss for people in their 30s and 40s. Deep infections can destroy tooth structure and surrounding bone, leading to extractions when root canal therapy or restorations are no longer viable.
Periodontal (gum) disease is another major cause; advanced periodontitis destroys the ligament and bone that anchor teeth. Trauma from sports or accidents also accounts for tooth loss in this age group, often requiring immediate assessment.
Less common but relevant causes include failed dental work (fractured restorations, root fractures) and congenital absence of some teeth that lead to complications over time.
How Bone Loss Progresses After Tooth Loss
When a tooth is removed, the alveolar bone that once supported it loses the mechanical stimulation it received through the tooth root. This begins a process called resorption: the bone height and width decrease, typically most rapidly in the first 6–12 months after extraction.
Loss continues at a slower rate thereafter, which can alter your bite, make neighboring teeth tilt or drift, and reduce options for implants without grafting. If you delay replacement, you may need bone grafts, sinus lifts (for upper back teeth), or alternative prosthetics because the ridge becomes too narrow or short for straightforward implant placement.
Identifying Risk Factors Unique to This Age Group
Your lifestyle and health in your 30s and 40s shape risk more than age alone. Smoking and poor oral hygiene accelerate both tooth and bone loss by increasing inflammation and impairing healing after extractions or surgeries.
Systemic conditions that often emerge or worsen in this decade—such as uncontrolled diabetes, hormonal changes, and certain autoimmune disorders—raise your risk of periodontal disease and slower bone healing.
Medication use matters too: drugs like bisphosphonates or some SSRIs can affect bone metabolism or healing after tooth removal. Finally, delayed treatment choices—opting to “wait” after extraction—raises the likelihood you’ll need more invasive bone-preserving procedures later.
Consequences of Delaying Treatment for Missing Teeth
Delaying treatment can cause progressive jawbone loss, changes in how your face looks, and practical problems with speech and eating. Each issue typically starts small but becomes harder to reverse the longer you wait.
Impact of Bone Deterioration on Oral Health
When a tooth is missing, the underlying jawbone no longer receives normal chewing forces and begins to resorb. Bone width and height can shrink within months to years, which reduces the bone available for future dental implants and can make dentures unstable.
Loss of adjacent bone also changes how neighboring teeth fit together. Teeth next to the gap can tilt or drift into the space, creating bite misalignment and increasing wear on other teeth. You may face a higher risk of gum recession and localized periodontal problems around shifted teeth.
If you plan implants later, significant bone loss often requires grafting procedures to rebuild volume. Grafting increases cost, treatment time, and complexity. Acting early preserves bone and keeps more straightforward restorative options available.
Changes in Facial Structure and Appearance
Bone loss under missing teeth affects the jaw’s vertical support and the soft tissues it holds up. You may notice a sunken appearance around the mouth, deeper nasolabial folds, or premature collapse of the lower third of the face. These changes can make you look older than you are.
Missing posterior teeth reduces vertical dimension of occlusion over time, which can cause the lower face to shorten and the chin to move closer to the nose. Lip support weakens, and wrinkles can become more pronounced. Non-surgical cosmetic fixes rarely address the underlying bone loss, so restorative dental work is the more effective route to restore natural facial contours.
Timely replacement preserves jaw height and facial proportions, limiting the need for more extensive dental and cosmetic procedures later.
Effects on Speech and Diet
A missing tooth in the front alters how air and tongue contact teeth, which can produce lisps or whistle sounds when you pronounce sibilants (s, z, sh). Even a single lateral incisor can change consonant production, causing social discomfort or the need to adjust speech habits.
In the back of the mouth, missing molars reduce chewing efficiency. You may avoid harder foods like raw vegetables, nuts, or meat, shifting your diet toward softer, often less nutritious choices. Uneven chewing increases stress on remaining teeth, raising the chance of fractures and TMJ pain.
Restoring missing teeth improves articulation and lets you chew across both sides evenly, protecting your remaining teeth and supporting a balanced diet.
Effective Solutions for Preventing Bone Loss and Restoring Your Smile
Act quickly to preserve jawbone volume, replace missing teeth, and protect adjacent teeth. The most effective approaches combine timely tooth replacement, targeted bone regeneration when needed, and a strict oral-care routine after restoration.
Early Intervention with Dental Implants
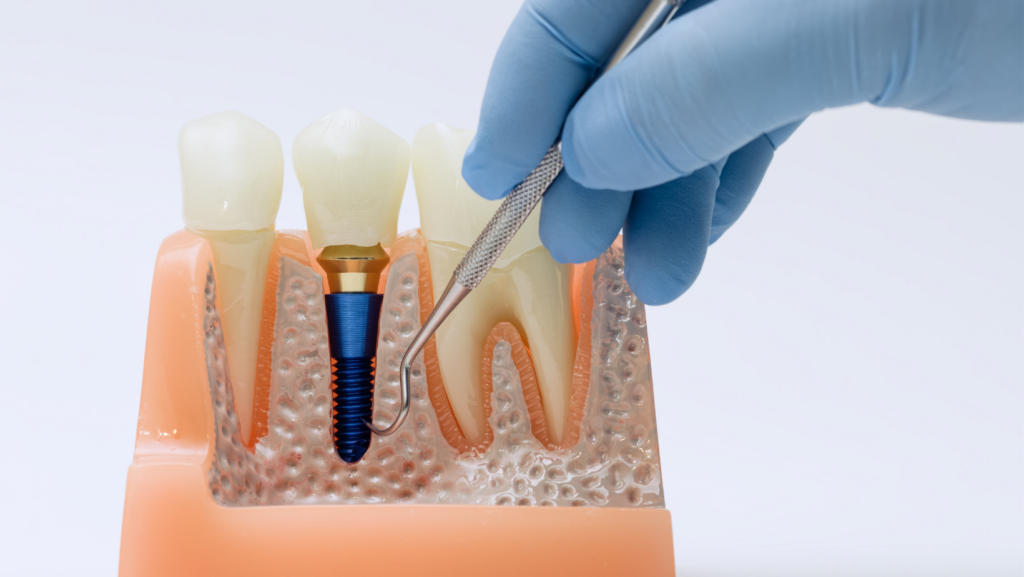
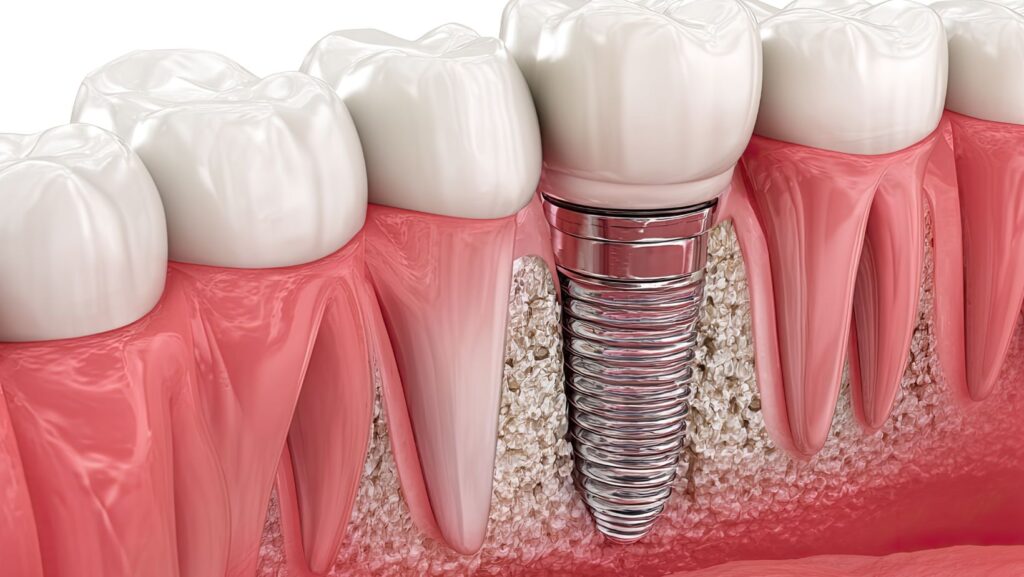
Dental implants replace tooth roots with titanium posts that stimulate bone through normal chewing forces. Placing an implant soon after extraction—often within weeks to a few months—limits bone resorption and preserves ridge height for future restorations.
You should get a CBCT scan and clinical exam to confirm sufficient bone and plan implant position. Immediate or early implant placement fits many cases, but your clinician may delay if infection or insufficient bone exists.
Benefits include long-term stability, prevention of adjacent tooth movement, and improved chewing efficiency compared with bridges or removable dentures. Discuss timing, implant diameter/length, and prosthetic plan (single crown, implant-supported bridge, or overdenture) to match your anatomy and lifestyle.
This dentist in Tampa FL adds that choosing dental implants serves as a vital safeguard for your facial aesthetics. By maintaining the natural density of the jawbone, this treatment prevents the premature facial sagging and sunken contours often associated with long-term missing teeth, allowing you to sustain a youthful appearance alongside a fully restored smile.
Bone Grafting and Regenerative Options
When bone volume is lost, grafting rebuilds the ridge to support implants. Your dentist may use autograft (your own bone), allograft (donor bone), xenograft (animal-derived), or synthetic grafts depending on defect size and healing needs.
Common techniques include socket preservation at extraction, lateral ridge augmentation for narrow ridges, and sinus lifts for upper back teeth. Growth factors (PRF/PRP) and barrier membranes can accelerate regeneration and improve graft integration.
Healing time varies: socket preservation often allows implant placement in 3–4 months; larger augmentations may need 4–9 months. Your provider will outline risks, success rates, and a staged timeline so you know when to expect implant placement.
Maintaining Oral Health After Tooth Replacement
Protect your investment with daily care and regular professional checks. Brush twice daily with a soft brush, floss or use interdental brushes around implant crowns or bridges, and use an antibacterial mouthwash if recommended.
Schedule dental cleanings every 3–6 months based on your risk level. Your clinician will assess peri-implant tissues for inflammation (mucositis) or bone loss (peri-implantitis) and intervene early with cleaning, topical antibiotics, or surgical treatment if needed.
Avoid smoking and control systemic factors like diabetes, as they increase implant and graft failure risk. Follow post-op instructions after surgery—nutrition, oral hygiene, and activity restrictions—to support predictable healing.