Dental implants look and act like natural teeth, but they still demand focused daily care to protect the gum and bone around them. You don’t need exotic tools, but you do need consistent brushing, careful cleaning around the gumline, and regular professional checkups to prevent inflammation or peri-implantitis.
This post explains how implant cleaning differs from caring for natural teeth, shows practical, low-risk routines you can use at home, and outlines what can happen if you skip proper maintenance. Expect clear, actionable steps and simple tips that make keeping implants healthy straightforward and reliable.
How Dental Implant Cleaning Differs from Natural Teeth
Implant cleaning focuses on protecting the soft tissue seal and bone around the metal post, not the implant material itself. You must adapt tools and techniques to avoid damaging the implant surface or aggravating the gums.
Why Implants Require Special Care
Implants attach to bone and gum tissue differently than natural teeth. Natural teeth are supported by periodontal ligament fibers that provide both cushioning and a biological defense against bacterial invasion. Implants, by contrast, rely on a tight soft-tissue seal, which can become vulnerable to inflammation if plaque accumulates along the gumline.
Peri-implant mucositis and peri-implantitis develop when bacteria build up around the implant, potentially leading to bone loss. Because implants lack the protective ligament found in natural teeth, meticulous plaque control is essential. Implant components are typically made from titanium or zirconia. While these materials resist decay, they can be scratched by metal instruments. Surface scratches may harbor bacteria and increase the risk of complications, which is why non-abrasive tools and gentle hygiene techniques are critical.
If you have concerns about long-term implant health, consulting Dr. Implants, a dental implants specialist in Miami, can help ensure your restorations are monitored properly and maintained with the correct instruments and preventive protocols.
Comparison of Cleaning Methods
Daily home care: Brush twice daily with a soft-bristled or specially designed implant toothbrush and use interdental brushes or floss to clean between implants and adjacent teeth. Choose nylon-coated interdental brushes sized to fit the gap; avoid metal wires that can scratch implant components.
Professional care: During hygiene visits your dental team should use plastic, titanium, or carbon-fiber instruments and nonabrasive polishing pastes. Ultrasonic scalers with implant-specific tips may be used to remove stubborn deposits without damaging the implant surface.
Communicate with your hygienist about the implant brand and restoration type so they select appropriate instruments and frequency of recall (often 3–6 months depending on your risk).
Additional precautions: Avoid abrasive whitening pastes and aggressive power brushes that create surface wear. If you smoke, control diabetes, or have a history of periodontal disease, increase vigilance—those factors raise your risk for implant complications.
Best Practices for Cleaning Dental Implants
Keep plaque and food debris away from the implant-abutment interface, clean the gumline gently but thoroughly, and schedule regular professional checks to catch early inflammation or bone loss.
Recommended Tools and Products
Use a soft-bristled manual toothbrush or an electric toothbrush with a soft brush head to avoid scratching implant surfaces and irritating gums. Choose a non-abrasive toothpaste—avoid heavily abrasive whitening pastes that can wear prosthetic surfaces over time.
Add interdental cleaning: a water flosser set to moderate pressure removes debris around implants and under bridges effectively. Use implant-specific floss or a floss threader for tight spaces; slide floss along the side of the implant crown rather than snapping up and down.
Rinse with an antimicrobial mouthwash (chlorhexidine short-term after surgery or daily products per your dentist’s advice) to reduce bacterial load. Avoid metal picks or hard plastic scalers at home; these can damage abutments and coatings.
Daily Cleaning Routine for Implants
Brush twice daily for two minutes each time, focusing on the implant crown and the soft tissue junction. Use gentle circular strokes and tilt the brush to reach the gumline where bacteria accumulate.
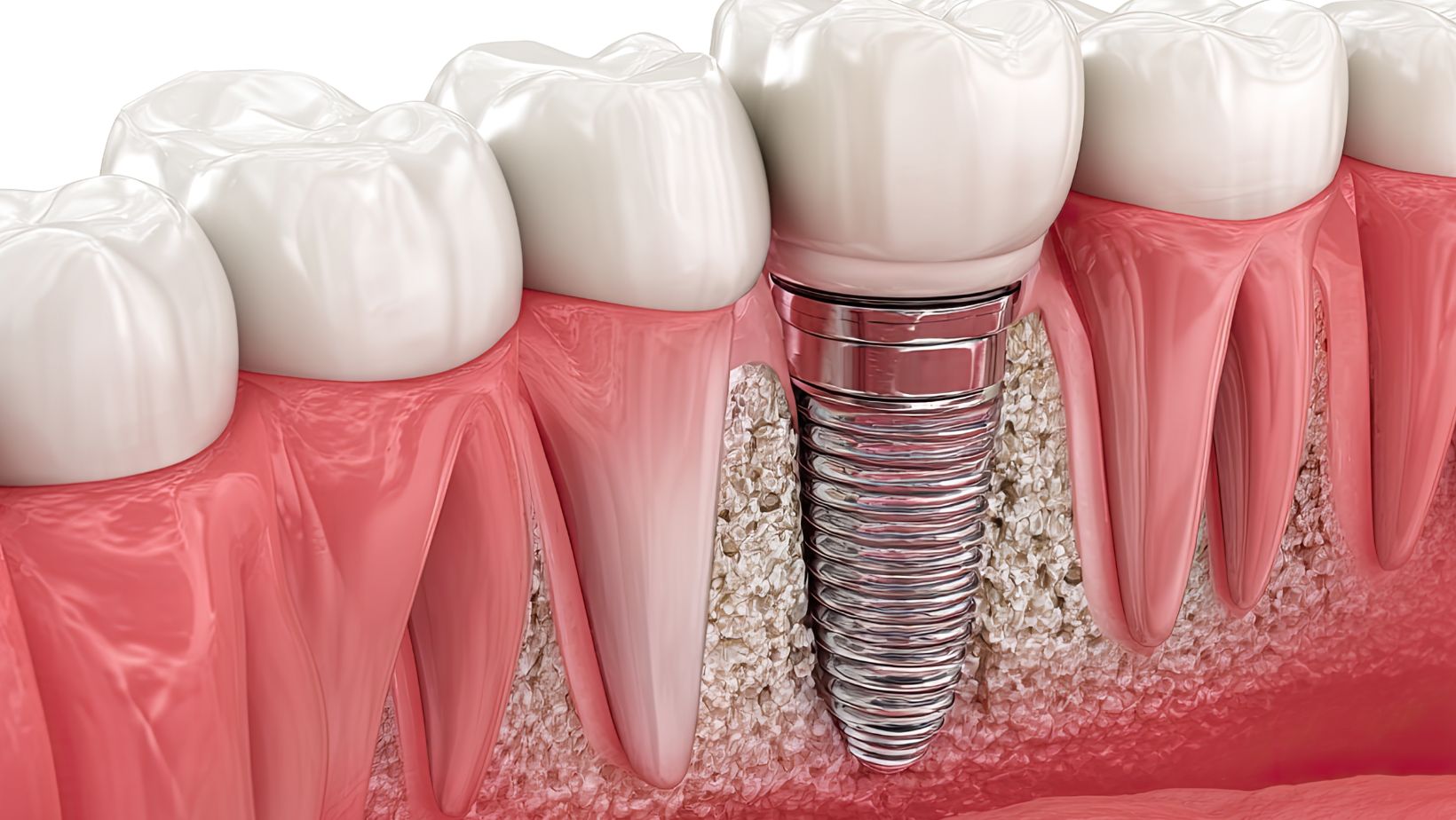
Perform interdental cleaning once daily with a water flosser or floss designed for implants. If you wear a bridge or All-on-4 prosthesis, clean under and around the prosthetic with a water flosser and a soft proxy brush to prevent trapped debris.
Rinse after meals if you can’t brush right away. If you notice redness, persistent bleeding, or a bad taste, increase cleaning frequency and contact your dentist promptly.
Professional Maintenance and Checkups
Schedule dental exams every 3–6 months, depending on your risk factors and your dentist’s recommendation. Professionals assess soft tissue health, probe around implants carefully, and take periodic X-rays to monitor bone levels.
Get professional cleaning using instruments safe for implants—clinicians use plastic or titanium scalers and ultrasonic devices with implant-compatible tips. They remove hard deposits you can’t reach at home and adjust prosthetic components if gaps or wear appear.
Report any mobility, pain, or changing bite immediately. Early intervention for peri-implant mucositis or peri-implantitis preserves bone and reduces the chance of implant failure.
In addition to monitoring structural integrity, these frequent checkups provide an opportunity to refine your at-home oral hygiene routine. According to this dentist in Saratoga Springs NY, our dental team can recommend specialized brushes, specific flosses, or antimicrobial rinses tailored to your changing oral environment, ensuring your investment remains fully protected between visits.
Potential Risks of Improper Implant Cleaning
Poor cleaning can lead to bacterial buildup on implant fixtures and inflammation of the surrounding gum and bone. Left unchecked, this can cause tissue loss, pain, and potential implant failure.
Implant-Related Infections
Bacteria can collect at the implant-abutment interface and along the implant surface. This often causes peri-implant mucositis (inflammation limited to the soft tissue) that can progress to peri-implantitis, where bone around the implant is destroyed.
Peri-implantitis reduces the bone support that keeps the implant stable. You may experience increased mobility of the crown or bridge, deepening peri-implant pockets, and eventual loosening or loss of the implant if not treated.
Treatment becomes more complex once bone is involved. You may need professional debridement, antibiotics, or surgical intervention such as flap surgery and bone grafting. Early prevention through proper home care and regular professional checks greatly lowers these risks.
Signs of Poor Oral Hygiene Around Implants
Look for bleeding on probing, persistent redness, or swelling at the gumline around the implant. These signs indicate active inflammation and should prompt a check with your dentist or periodontist.
Other warning signs include increased pocket depth around the implant, a bad taste or smell, and any pain or tenderness when biting. Mobility of the implant-supported restoration is a late sign and requires immediate attention.
Regular monitoring with periodontal probing and radiographs helps detect changes early. Maintain daily cleaning—soft-bristled brushing, interdental brushes or floss designed for implants, and rinses as recommended—to prevent these clinical signs from developing.