Sitting behind a laptop for hours, hopping between client calls, or running campaigns across time zones are familiar routines for online business owners and SEO professionals. But long periods of sitting or standing can contribute to leg swelling, aching, and visible varicose veins. At Metro Vein Centers, patients can access expert evaluation and treatment for these issues, combining minimally invasive procedures with evidence-based care to restore comfort and circulation. This article explains how to recognize problematic symptoms, how specialists diagnose varicose veins, immediate self-care steps, the medical and procedural treatments available, and practical guidance for choosing the right specialist. It’s designed to help busy marketers and agency owners identify when conservative measures aren’t enough and take actionable steps toward lasting relief.
Recognizing When to See a Varicose Vein Specialist
Common Symptoms and Causes of Swelling and Pain
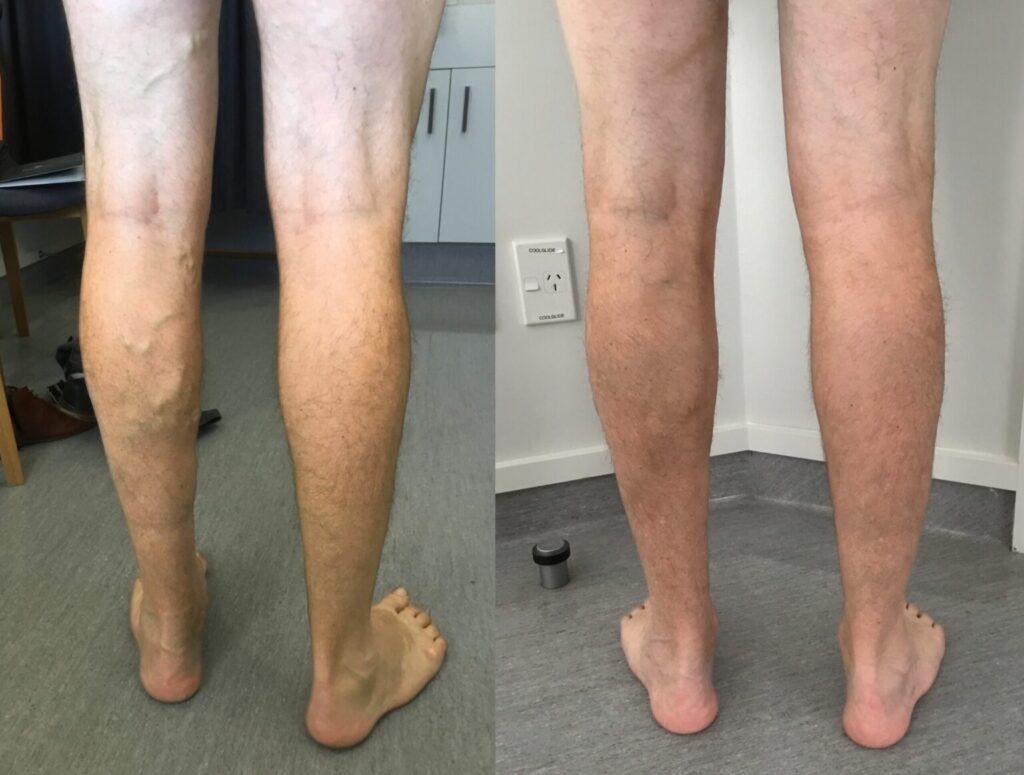
Varicose veins are enlarged, twisting veins visible under the skin, most commonly in the legs. Symptoms that commonly prompt a visit to a specialist include:
- Persistent aching, throbbing, or heaviness in the calves or thighs.
- Swelling in the ankles or lower legs that worsens when days end.
- Visible bulging veins, blue or purple discoloration, or clusters of small spider veins.
- Itching, burning, or skin changes (dryness, thinning, or discoloration) around the affected area.
- Restless legs or pain that interferes with sleep, mobility, or daily work.
The underlying causes are often related to venous insufficiency: weakened or damaged valves inside leg veins allow blood to pool rather than return efficiently to the heart. Prolonged sitting, standing, hormonal changes, pregnancy, age, genetics, and obesity all contribute to increased venous pressure and the formation of varicosities.
Risk Factors that Worsen Symptoms
Certain factors increase both the risk of developing varicose veins and the likelihood that symptoms will progress:
- Prolonged immobility: long workdays spent seated at a desk or standing at events make it harder for calf muscles to pump blood upward.
- Age: vein valves lose strength over time.
- Family history: a strong genetic component makes some people predisposed.
- Hormonal changes: pregnancy or hormonal therapies can weaken vein walls.
- Obesity: extra weight increases venous pressure in the legs.
- Prior deep vein thrombosis (DVT) or leg injury: these can damage valves and circulation.
For online entrepreneurs who work long hours, especially those who also travel frequently, the combination of sitting and stress can accelerate symptom onset. When swelling and pain become recurring or progressive rather than occasional, it’s time to consult a specialist rather than relying solely on home remedies.
How Specialists Diagnose Varicose Veins
Physical Exam and Symptom Assessment
The first step with a varicose vein specialist is a focused medical history and physical exam. The clinician will ask about the pattern of symptoms, triggers, family history, prior blood clots, pregnancies, and any skin changes. Observation while standing helps reveal refluxing veins and areas of swelling. A careful exam distinguishes cosmetic spider veins from deeper venous insufficiency that requires treatment.
Short-Term Relief Strategies You Can Try Now
Compression Therapy and Elevation Techniques
Compression stockings remain a mainstay for immediate symptom relief. Graduated compression improves venous return, reduces swelling, and relieves aching. A specialist or certified fitter can recommend the appropriate compression level (measured in mmHg) and style for the patient’s daily routine.
Elevating the legs above heart level for 15-30 minutes a few times daily helps fluid drain from the lower extremities. For busy professionals, short elevation breaks, lying back on a couch with legs propped on pillows, can reduce end-of-day swelling and restore comfort.
Lifestyle Changes and At-Home Measures
Several practical habits reduce symptoms and slow progression:
- Break up long sitting or standing periods by walking for several minutes each hour.
- Use a standing desk periodically: alternate sitting and standing.
- Maintain a healthy weight and follow a low-sodium diet to limit fluid retention.
- Wear comfortable shoes and avoid tight clothing that restricts circulation.
- Incorporate a calf-strengthening exercise (heel raises, ankle pumps) into a short daily routine.
For marketers and agency leads, integrating movement into workflows, walking meetings, scheduled activity reminders, or brief stretch breaks can be both productivity-friendly and therapeutic.
When to Use Medication or Pain Management
Over-the-counter NSAIDs can relieve inflammatory pain temporarily, but they don’t treat the underlying venous insufficiency. For neuropathic or severe pain, a specialist may prescribe short-term pain control or refer to a pain-management protocol.
Topical agents and venoactive drugs (available in some countries) may offer symptomatic relief, but evidence varies. A specialist will advise on medical options and align them with plans for definitive procedures if indicated.
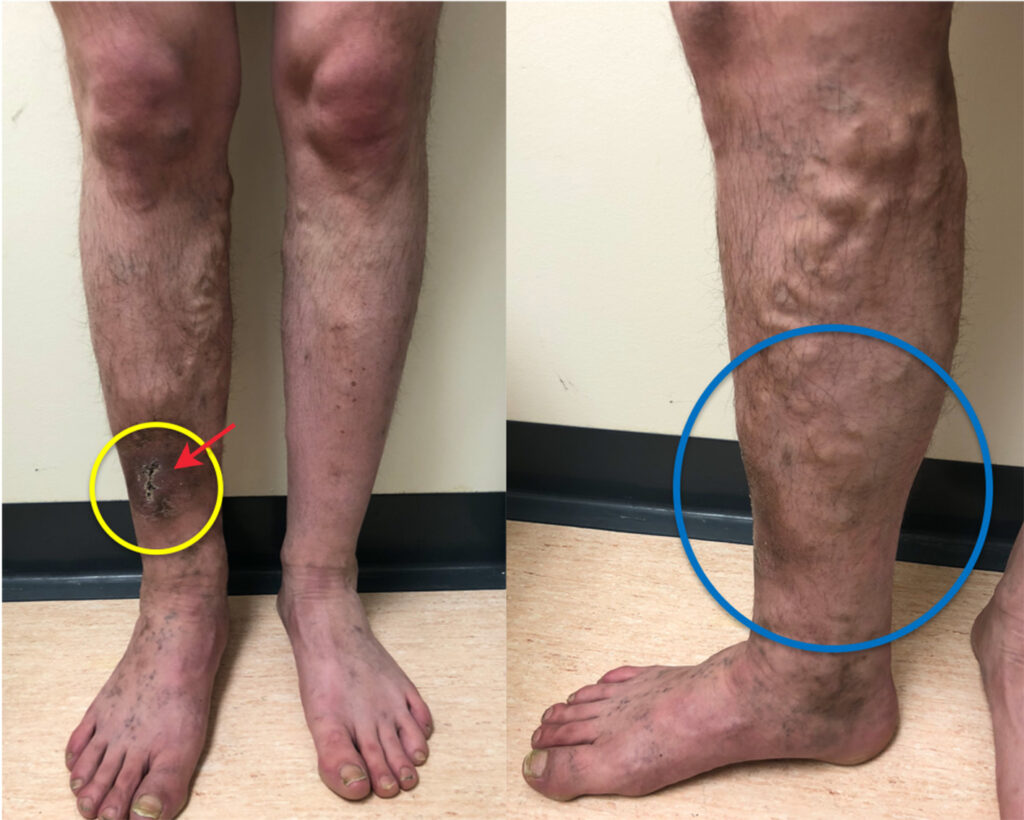
Medical and Procedural Treatment Options Offered by Specialists
Minimally Invasive Procedures (Ablation, Sclerotherapy, Phlebectomy)
Modern varicose vein treatment emphasizes minimally invasive procedures that provide durable symptom relief with less recovery time than traditional surgery:
- Endovenous Ablation (thermal or laser): A catheter delivers heat (radiofrequency or laser) to seal the incompetent vein. Local anesthesia is typical: patients often return to light activity the same day.
- Ultrasound-Guided Foam Sclerotherapy: A sclerosant injected into refluxing veins causes closure and gradual resorption; it works well for branching veins and some larger trunks.
- Ambulatory Phlebectomy: Small incisions remove surface varicosities under local anesthesia. It’s effective for prominent bulging veins with excellent cosmetic results.
These procedures are often combined in a single session, treating the primary reflux source and removing symptomatic tributaries, yielding both functional and visible improvement.
Expected Recovery, Risks, and Outcomes
Recovery from minimally invasive procedures typically involves mild bruising, temporary numbness, and mild discomfort for a few days to weeks. Compression use and short walking are encouraged post-procedure. Serious complications are uncommon but can include infection, blood clots, nerve injury, or skin changes. Long-term outcomes are favorable for most patients: reduction in pain and swelling, improved mobility, and better cosmetic appearance.
A realistic expectation and shared decision-making are central: specialists outline success rates, possible need for staged treatments, and follow-up plans to monitor recurrence or new symptoms.
Choosing the Right Varicose Vein Specialist
Credentials, Experience, and Procedure Volume to Look For
Selecting a specialist matters. Patients should seek clinicians board-certified in vascular surgery, interventional radiology, or phlebology with focused training in venous disease. Experience, measured in procedure volume and years treating venous insufficiency, correlates with consistent outcomes.
Look for clinics that perform duplex ultrasound in-house and publish outcome data or patient testimonials. A multidisciplinary team (vascular surgeons, interventionalists, ultrasound technologists) often signals comprehensive care.
Questions to Ask During Your Consultation
During the first visit, patients should come prepared with specific questions:
- Which veins are causing my symptoms, and how will you diagnose them?
- What treatment do you recommend and why? Are there alternative options?
- What are the risks, expected recovery time, and success rates for this treatment?
- Will the procedure be done in-office, outpatient, or hospital? What anesthesia is used?
- How many similar procedures have you performed, and can I see before/after photos or outcomes data?
These questions help busy professionals assess efficiency and likely return-to-work timelines, important considerations for entrepreneurs balancing health and business demands.
Insurance, Cost Considerations, and Treatment Planning
Insurance coverage varies: many insurers cover treatment when venous insufficiency causes medically significant symptoms (swelling, ulceration, pain), but not for purely cosmetic concerns. A reputable clinic will assist with preauthorization, provide clear cost estimates, and outline staged treatment plans aligning with insurance criteria.
Patients should discuss downtime, phased procedures, and follow-up visits so they can plan client work, campaigns, or travel around treatment and recovery.
Conclusion
Varicose veins are common and often manageable, but persistent swelling and pain merit specialist assessment, especially for professionals whose work patterns (long sitting, travel, shift work) elevate risk. A varicose vein specialist combines careful diagnosis with a range of evidence-based options: from compression and lifestyle adjustments to minimally invasive ablation and targeted phlebectomy.
For time-pressed entrepreneurs and agency leaders, the right specialist not only relieves symptoms but also helps plan treatment around business needs. Choosing a credentialed clinician who uses duplex ultrasound, explains expected outcomes, and offers clear cost guidance ensures efficient, effective care that gets people back to work and comfortably on their feet, so they can focus on growth rather than swelling and pain.